Gastroenterology
Comprehensive GI Pathology Services
Gastroenterologists & Primary Care Providers
LabGenomics provides a full range of GI tests and pathology services focused on supporting your screening, diagnostic and case management strategies. Our pathologists are ready to collaborate with you on identifying the right pathway forward for successful clinical outcomes.
Our GI pathologists provide expert interpretation of a full range of cases that focus on the diagnosis and characterization of neoplastic and non-neoplastic diseases with special emphasis on chronic inflammatory diseases and tumors in the GI tract, pancreas and liver.
- Fellowship Trained GI pathologists:
LabGenomics staff GI pathologists are fellowship trained in GI and liver pathology and have special interest in Pediatric GI pathology.
- Personal Consultation:
Our pathology staff provides personal consultation with the ordering physician on unusual cases upon request.
- Interpretive Reports:
Images and graphic reporting elements are included in the final report which aids in the understanding of the findings.
Our GI pathologists provide expert interpretation of a full range of cases that focus on the diagnosis and characterization of neoplastic and non-neoplastic diseases with special emphasis on chronic inflammatory diseases and tumors in the GI tract, pancreas and liver.
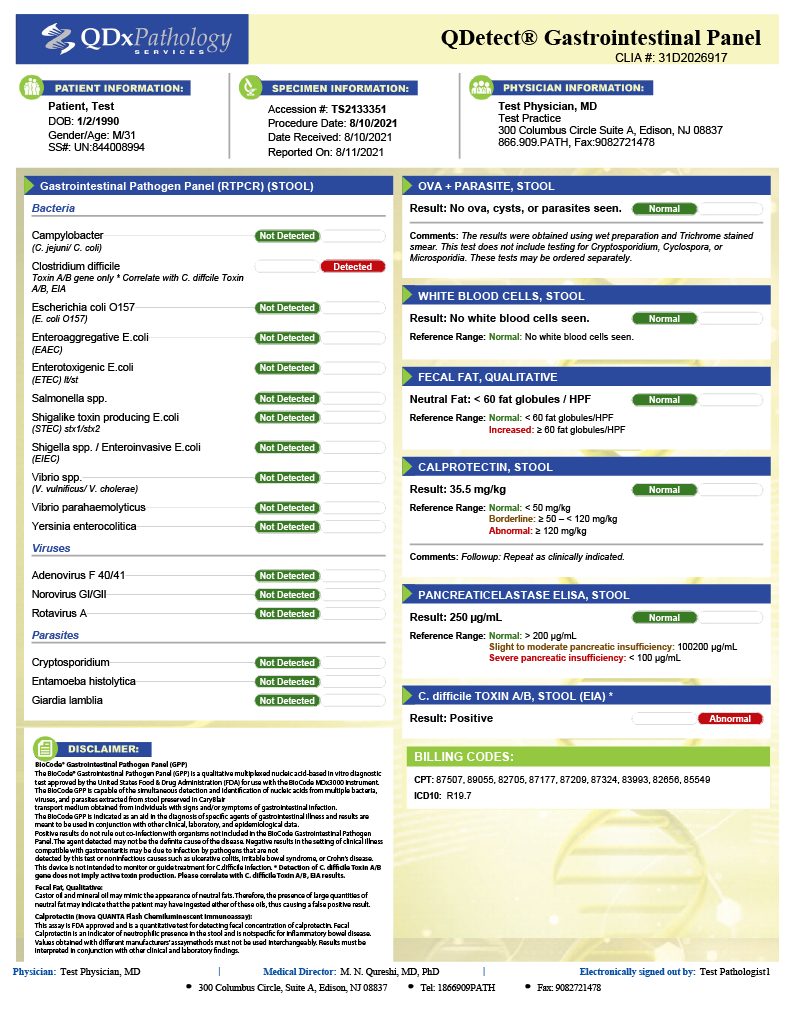
GI Pathogen Panel is based on multiplexed nucleic acid detection and is intended for the simultaneous qualitative detection and identification of multiple viral, bacterial and parasitic nucleic acids in human stool samples. This includes Cary-Blair media from individuals with signs and symptoms of gastrointestinal infection.
Turn Around Time – 48 hours.
Clostridium difficile infection involves a range of clinical presentations from mild diarrhea to life-threatening pseudomembranous colitis and megacolon. Moderate to severe CDI cases require early identification for better outcomes and decreased mortality. Especially among the elderly.
Turn Around Time – 24 hours.
H. Pylori is responsible for 90% of duodenal ulcers and 80% of gastric ulcers. It is also associated with a 2-3 fold increased risk of gastric cancer and mucosal associated-type (MALT) lymphoma.
H. pylori stool antigen is a qualitative test that detects Helicobacter pylori specific antigen. It is intended for use with human fecal specimens to aid in the diagnosis of H. pylori infection and to demonstrate loss of H. pylori antigen following treatment.
Turn Around Time – 48 hours.
Our stool testing services support the determination of the underlying causes of gastrointestinal illnesses (bacteria, parasites), as well as diseases, such as colitis or inflammatory bowel disease.
Fecal Fat
Fecal fat measures the amount of fat within a stool sample. Excess fat known as steatorrhea can be tested for this, ultimately aiding in the determination of malabsorption and/or digestive disease. We test for both the presence of neutral fats and split fats in stool. Neutral fats (e.g., monoglycerides, diglycerides, triglycerides) seen in excess is suggestive of steatorrhea, impaired synthesis or secretion of pancreatic enzymes or bile. An increase in split fats is suggestive of impaired absorption of nutrients. These neutral/split fats should be rare in normal stool samples.
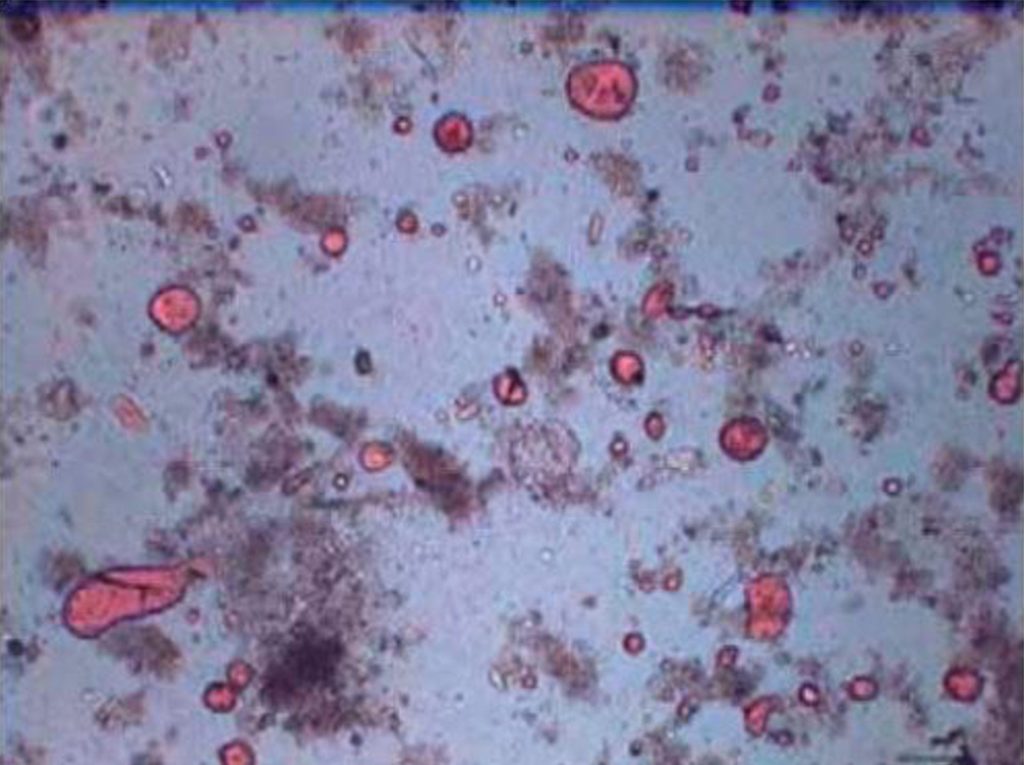
OVA AND PARASITES SCREENING TEST
The Ova and Parasite stool test is a microscopic exam to help diagnose the appearance of eggs, trophozoites and/or helminths found within stool. Parasitic infections often occur in the lower digestive tract, which may cause diarrhea.
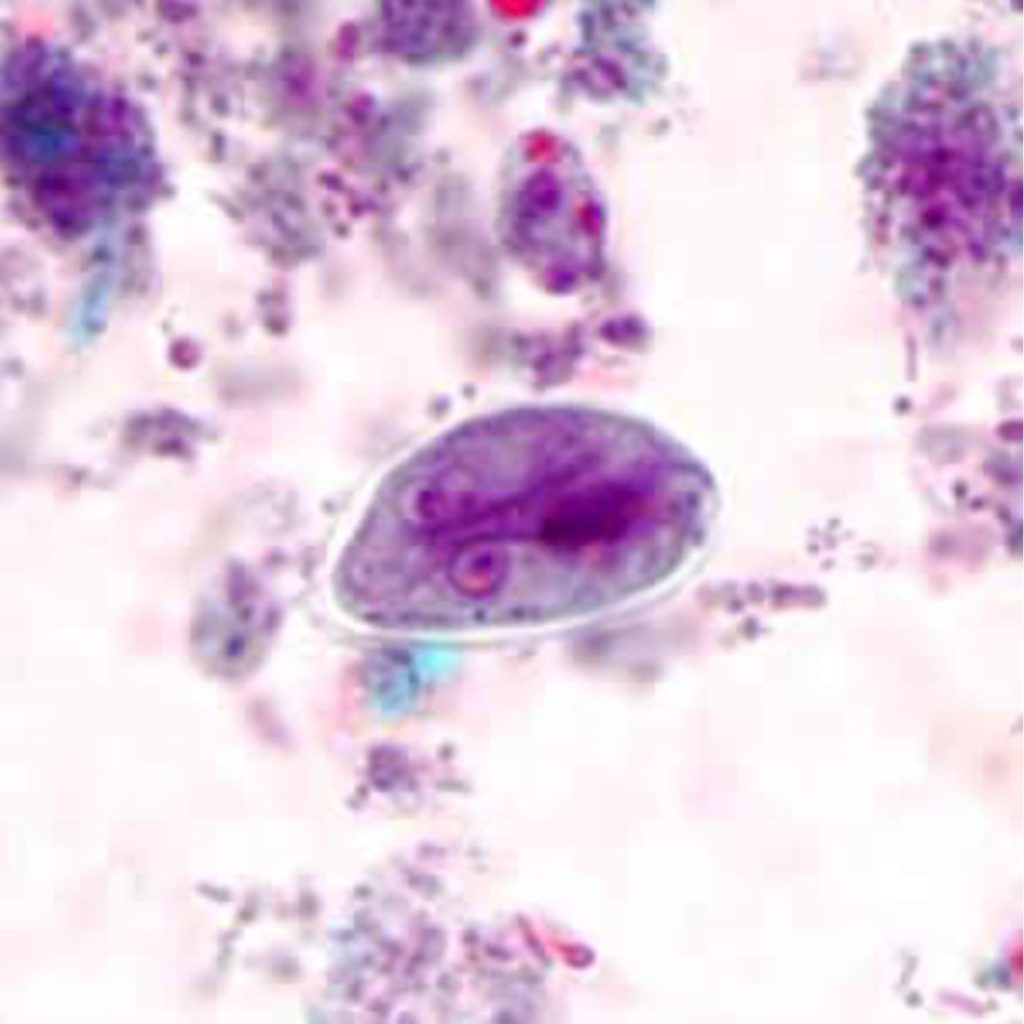
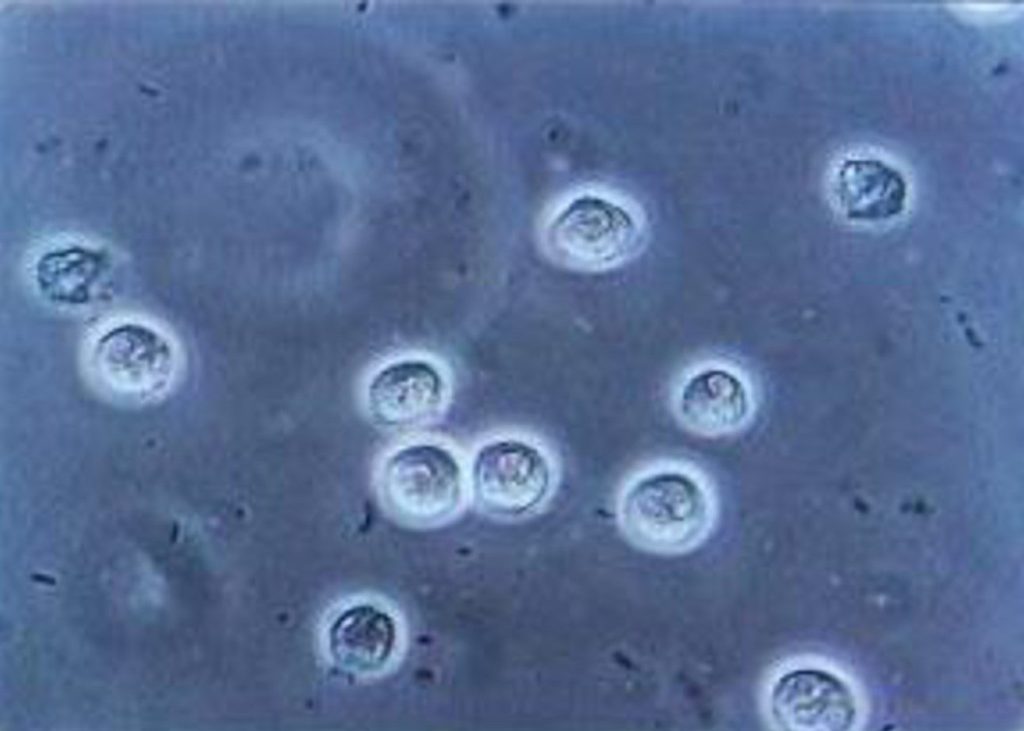
FECAL WHITE BLOOD CELL (WBC) STOOL TEST
White Blood Cell stool testing or Fecal Leukocyte testing help diagnose inflammatory diarrhea. This type of diarrhea may be an indication of an infection by bacteria, or the result of ulcerative colitis or inflammatory bowel disease.
Note: If ordering Calprotectin or Lactoferrin, Fecal WBC is of limited value and should not be ordered.
LabGenomics offers several immunoassays to detect the presence of blood, bacteria or parasites, as well as other signs of diseases and disorders. Our laboratory utilizes advanced analytic methods and equipment including chemiluminescence immunoassays that improve detection sensitivity when compared to standard immunoassays.
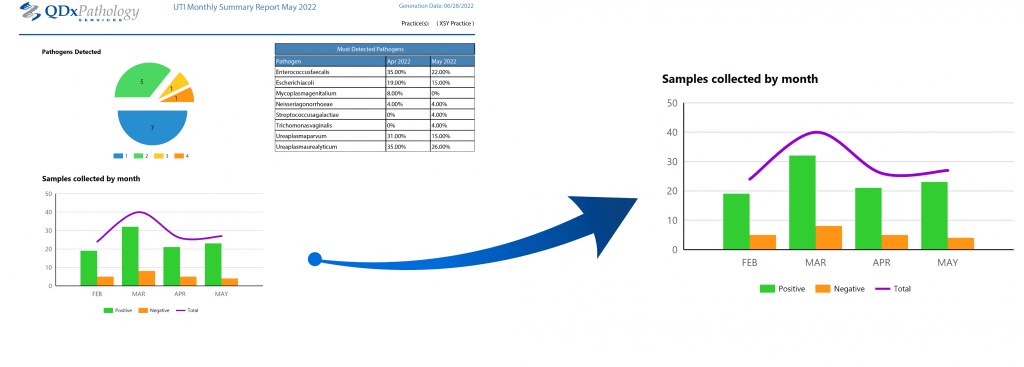
Clinical Management Report
Upon request, LabGenomics provides your practice with clinical management reports that summarize aggregate test result data to support your quality assurance process. Contact your LabGenomics representative to learn more.